24 Nursing Trends We Expect to See in 2024
by Carson-Newman … on May 19, 2021
Updated January 18, 2024.
We've put together a list of top nursing issues and trends that we expect to see in 2024 and beyond based on the latest data and insights from American Nurse Today, the Association of American Medical Colleges (AAMC), the American Association of Nurse Practitioners (AANP), and other sources.
The medical field, particularly nursing, is still experiencing the long-term effects of the COVID-19 pandemic. As the current field of nurses becomes more educated, they have an opportunity to take on expanded roles and fill a drastic need in the years to come. Read on to learn what to expect in the ever-changing world of nursing in 2024.
Why It's Important to Stay Ahead of Nursing Trends and Issues
Why should health care professionals stay abreast of future trends in nursing? By monitoring nursing issues and trends, nurses can:
- Become better advocates for patient safety, comfort and care
- Apply cutting-edge technologies to optimize efficiency and improve outcomes
- Safeguard their own mental health and well-being
- Collaborate with other nurses, doctors and specialists more ably
- Seize opportunities for nurse leadership, including heightened responsibility and more competitive pay
These are just a few of the many benefits of keeping up with future trends in nursing. Here are some of the top nursing trends for the coming year.

1. Online Education Programs Will Continue to Increase in Popularity
In 2010, the Institute of Medicine (IOM) appointed the Committee on the Future of Nursing to put together recommendations for an action-oriented response to some of the challenges nurses are facing.
One of its key recommendations was to increase the percentage of workers holding a Bachelor of Science in Nursing (BSN) degree from 50% to 80% by 2020. In 2018, New York became the first state to pass a law requiring nurses to earn a BSN within ten years of becoming licensed. Many other states have plans to adopt similar legislation.
In light of these changes, the motivation for nurses to pursue higher education is stronger than ever. Online nursing degree programs provide a way for nurses to obtain a degree while continuing to work full time, opening the door to higher education without sacrificing work-related responsibilities or family obligations.
We predict the popularity of online Master of Science in Nursing (MSN) to Family Nurse Practitioner (FNP) and online Post-Master's FNP Certificate programs to increase in 2024 as virtual education evolves from a pandemic necessity to a mainstay for career advancement.
2. The Shortage of Primary Care Physicians Will Create an Even Greater Demand for Family Nurse Practitioners
Recent research from the AAMC found that the United States could face a shortage of up to 48,000 primary care physicians by 2034 due in part to a growing aging population.
Without enough primary care physicians to care for the population, the demand for family nurse practitioners (FNPs) will be high, especially in those states where they have full practice authority. In November 2023, AANP reported that the United States had 385,000 licensed nurse practitioners (LNPs). We expect this number to continue to grow.
Another factor in the increasing demand for FNPs is rural hospital closings, which significantly impact health care. Between 2010 and 2021, a total of 136 of all rural hospitals closed their doors, according to the American Hospital Association (AHA). This is undoubtedly one of the most significant nursing trends of the last several years.
About 14% of the U.S. population, or 46 million people, live in rural areas and already find it challenging to obtain health care, according to the AHA. Another issue impacting residents in these areas is the insufficiency of doctors. FNPs can perform checkups, physicals, etc. for patients who might otherwise be stuck waiting long periods of time for an appointment with a doctor.
Earn Your MSN-FNP Part-Time For Less than $30k
3. A Greater Number of States Will Grant Nurse Practitioners Full Practice Authority
As a further response to the primary care physician shortage, more states are likely to grant nurse practitioners (NPs) the authority to practice independently. Currently, about 30 states and U.S. territories grant NPs full practice authority, while other states require collaborative agreements with supervising physicians or have practice restrictions.
Given the pressing need for primary care providers and the fact that both the National Academy of Medicine (NAM) and the National Council of State Boards of Nursing (NCSBN) recommend that states provide NPs full practice authority, the remaining states face increasing pressure to follow suit.
Learn how COVID-19 has impacted NP practice authority.

4. We Will See Significant Job Growth for Nurses in 2024
The numbers are clear: In the U.S. and globally, the shortage of registered nurses (RNs) is expected to intensify as baby boomers age, the need for care providers grows and health care workers deal with the long-term effects of COVID-19.
The nursing shortage intensified due to the COVID-19 pandemic as hospitals and other health care environments struggled under unprecedented patient loads.
The U.S. Bureau of Labor Statistics (BLS) projects registered nursing to be a fast-growing profession through 2032. The BLS expects it to grow by 6%; an estimated 177,400 new RN jobs will be added by 2032.
This demand stems from the United States having an aging population. By 2030, the U.S. Census Bureau states that 21% of the population will be of retirement age. By 2034, there will be more people over age 65 than those under 18. It's expected that there will be a 48,000-plus shortage of primary care physicians by 2034, with many of today's doctors retiring. An aging population will need access to medical professionals, and FNPs are equipped to help fill this void
The lack of nurse educators is another issue. An AACN report explains that "U.S. nursing schools turned away 91,938 qualified applications from baccalaureate and graduate nursing programs in 2021 due to an insufficient number of faculty, clinical sites, classroom space, clinical preceptors and budget constraints."
5. Salaries for Registered Nurses Will Stay Steady or Increase
Despite COVID-19's negative impacts on inflation and hospital finances, nurses surveyed by the American Nurse Journal report that they've continued to receive salary increases. The rise in nurses' salaries is especially true for FNPs, whose median annual pay in 2022 was $121,610, according to the BLS. Medical facilities are also using other incentives to entice nurses. Many facilities are offering bonuses to both recruit and retain nurses.

6. More States Will Join the Enhanced Nurse Licensure Compact, Making It Easier for Nurses to Move Across State Lines
The enhanced Nurse Licensure Compact (eNLC) was officially implemented on January 19, 2018. The compact, coordinated by NCSBN, makes it substantially easier for travel nurses to work across state lines.
In 2023, Washington and Rhode Island became the latest states to sign the compact's provisions into law, bringing the total number of states and territories that have enacted and implemented the eNLC to 41.
7. Telehealth and Chatbot Services Are Making It Easier for Patients to Access Care
The coronavirus pandemic accelerated the demand for virtual health care. A 2022 U.S. Department of Health and Human Services (HHS) report found that 22% of respondents had telehealth appointments in the previous month. That's why we predict telehealth and chatbot services will continue to be the norm in some aspects of the nurse's role in 2024. This is among the clearest and most consequential future trends in nursing.
With telehealth technology, patients can manage certain aspects of their own health care by accessing an online portal to see their test results, schedule appointments and request prescription refills. Virtual appointments enable them to see their nurse or doctor via live video feed.
Similarly, chatbots can assist patients with things like booking appointments and reminding them to take certain medications. For example, the health care chatbot Florence monitors patients' health, gives patients instructions and reminders for taking pills, and helps patients find specialists in their area.
Telehealth has faced some legislative restrictions regarding Medicare payments in the past. As the rules related to payments and other regulations are eased, barriers to its growth will be lessened.
The relaxation of rules around reimbursement for telehealth visits in the wake of COVID-19 has shown health care providers and patients alike how well the systems can work.
Besides working for patients with minor complaints, telehealth visits are a boon for nurses, therapists and providers who can use the technology to manage patients with mobility challenges and who are at especially high risk if exposed to the coronavirus.
Read our blog to learn more about how FNPs use telehealth today.

8. Virtual Technology Will Also Help Practitioners
Virtual technology has already assisted nurses with many tasks and will continue to do so into 2024. Virtual assistants can help nurses make data-informed decisions about treatments and medications. It can also help improve health outcomes by reminding patients to take medication, automating prescription refills, and handling billing and insurance, which can free up time for nurses.
Virtual reality (VR) can also provide many opportunities for working nurses and nurse education simulations. Practitioners have recently begun to use VR for chronic pain management in patients, which has been linked to higher quality of life and fewer visits to the hospital. These emerging examples are just some of the potential opportunities for VR to assist nurses in 2024.
9. Bilingual Nurses Will Be More Valued
The U.S. population is becoming increasingly diverse. The U.S. Census Bureau reported that at least 350 languages are spoken in American homes as of 2023.
Next to English, Spanish is the most widely spoken language in the United States. An estimated 42 million U.S. residents, approximately 13% of the population, speak Spanish at home — more than twice as many as in 1990.
Bilingualism is becoming increasingly valued as a skill for nurses to have. Nurses who speak a second language, especially Spanish, may be more attractive to employers than monolingual nurses in 2024.
10. More Nurses Will Choose to Specialize
Nurses today are expected to specialize, a nursing trend likely to continue into 2024 and beyond.
Nursing is a career with greater demand at higher levels of practice than entry-level ones. Nurses who choose to specialize find that they're in higher demand and that they can command higher salaries.
The BLS reports that RNs had a median annual salary of $81,220 in 2022, with projected job growth of 6% between 2022 and 2032. However, NPs will enjoy even brighter prospects for employment and salary. According to the BLS, they earned a median annual wage of $121,610 in 2022, and their employment is projected to grow by 45% between 2022 and 2032.
From family health to psychiatry, nurses can choose to focus their careers on many advanced specialties in 2024.

11. More Focus Will Be Placed on Holistic Care
Holistic care is a method for treating the whole patient. Holistic nurses recognize each patient's unique physical, mental, emotional, spiritual and environmental strengths and weaknesses.
The global body of evidence about the benefits of holistic care is growing, placing it at the center of future trends in nursing.
A 2020 study of patients in Hong Kong found that those who received holistic care intervention reported better outcomes than patients who received routine care.
Increasingly, U.S. hospitals and other health care facilities are emphasizing integrative and holistic health in their delivery models. At Carson-Newman University, our online MSN-FNP and online Post-Master's FNP Certificate programs focus on holistic care.

12. Nurses With Technological Skills Will Be in High Demand
Technology is ever-present in the modern world of health care, and the pace of reliance on technology only increased with the COVID-19 pandemic. Nurses today use a wide range of technologically driven approaches to increase efficiency, including electronic health records (EHRs) to track health history and smart beds to optimize patient positioning.
Nurses' use of mobile devices is also rising. A Zebra Technologies study, the Future of Healthcare 2022 Hospital Vision Study, predicted that the percentage of bedside nurses who used mobile devices in their practice would increase from 65% in 2017 to 97% in 2022. The same study showed that mobile technology can improve cost savings, care quality and patient safety.
Technology in nursing is here to stay, and nurses will need to become confident and comfortable with it at an increasing pace.

13. The Field of Health Informatics Will Become More Mainstream
In response to the influx of health care technology, a new field has arisen: health informatics. This growing specialization uses data collected by information technology (IT) systems to create a more collaborative environment between patients and their various health care providers.
One survey by the Healthcare Information and Management Systems Society (HIMSS) found that respondents reported a direct positive impact on the quality of care patients received as a result of the work of informatics nurses. With a high average salary and a very good job outlook, this specialization should attract even more interest in 2024.

14. Patients Will Continue to Become More Educated
In the era of smart devices, people are constantly consuming more information, including health-related information. Nurses can now expect to see patients who've already researched their conditions or symptoms online and may have an understanding of which medications might be right for them based on pharmaceutical advertisements they've seen.
Nurses in 2024, especially NPs, must be prepared to serve a more educated patient population by listening to patients' views about their health condition and synthesizing this information with their own professional knowledge and expertise.
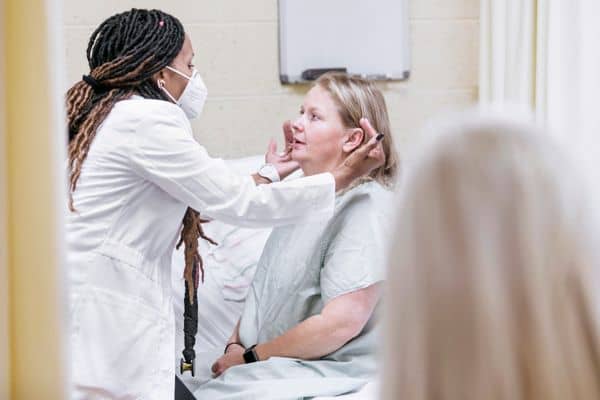
15. We'll See an Increase in Cost-Effective Urgent Care Clinics
The lines between the retail and health care industries are blurring. Retail health clinic services offered by major players, such as Walgreens and CVS, provide alternative channels for the provision of primary care. They're majorly disrupting the health care landscape.
Future Market Insights (FMI) estimates an annual growth rate of 9.6% in the global market for retail clinics through 2028. Researchers point to patient accessibility and affordability in explaining this growth.
This is good news for NPs, as many NPs have already opted to open up their own clinics within such retail locations.

16. Nursing Faculty Positions Will Become More Attractive
The demand for RNs may be growing, but paradoxically, many institutes of higher education have been forced to turn away qualified applicants due to an ongoing nursing faculty shortage.
According to an AACN report on enrollment and graduations in baccalaureate and graduate programs in nursing, U.S. nursing schools had to turn away 78,191 qualified applicants from baccalaureate and graduate nursing programs in 2022. AACN identifies budget and faculty constraints as factors contributing to the shortage.
In response to this crisis, many initiatives are underway to make nursing faculty positions more attractive to qualified nurses. One example of such an initiative is the Jonas Nurse Leaders Scholar Program, which provides financial support to more than 1,400 scholars in all 50 states to expand the pipeline of future nursing faculty.

17. The Demand for Geriatric Specialists Will Continue to Rise
America is aging, and that can't help but affect nursing issues and trends. The Congressional Budget Office (CBO) calculates that by 2060, 23% of the U.S. population will be 65 or older. In the coming years, more geriatric nurses will be required to deal with an aging and ailing population of baby boomers. New nurses entering the field in 2024 may wish to be at the forefront of this highly sought-after specialty by becoming certified in geriatric care management.

18. More Awareness Will Be Given to Common Issues Faced by Nurses
According to a 2023 McKinsey & Co. report, 31% of nurses are considering leaving their jobs. The reasons for this potential exodus are exemplified in a 2021 AMN Healthcare survey of RNs:
- High levels of stress at work
- Concerns about work-life balance
- Difficulty recovering from the emotional toll of work
- Impact of work on physical health
There's some good news to counter this nursing trend. AMN Healthcare found that 64% of nurses were likely to encourage others to join the profession, and 66% were likely to stay with their current employers. They believed in the work they were doing and its value to the world.
The awareness of nursing issues increased in 2022 and 2023. More organizations, such as the American Psychiatric Nurses Association (APNA), emphasize the importance of self-care to guard nurses against the effects of job-related stressors. As health care facilities work to retain nursing staff, more resources will be devoted to nurses' well-being and job satisfaction.
Read our blog on how to practice self-care as a nurse during COVID-19.
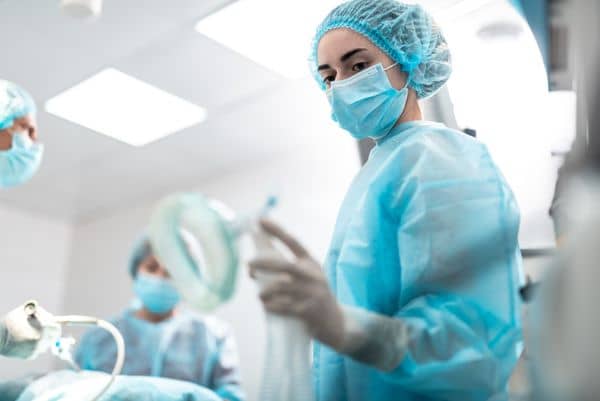
19. Nurses Will Continue to Retire Later
While the U.S. faces a nursing shortage, older nurses are delaying retirement. The number of nurses 65 and over increased from 14.6% in 2017 to 19% in 2021. That's according to the 2020 National Nursing Workforce Study conducted by NCSBN and the National Forum of State Nursing Workforce Centers.
Amid the coronavirus pandemic, some retired nurses started working again. In March 2020, HHS urged states to relicense retired health care workers for quick reentry into the workforce.
The trend toward later retirement is expected to continue in 2024 and beyond. What does this mean for new nurses entering the field? There will be many job opportunities as new nurses work alongside experienced colleagues.

20. Nurses Will Help Uphold Health Care Cybersecurity
With the increasing adoption of digital technologies in health care, such as multi-cloud infrastructure and telehealth, the risk of cyber threats also rises. Health care facilities will need to develop and implement strategies to mitigate potential cyberattacks that could compromise confidential information.
Because they upkeep patient records and serve as points of communication between patients and other health care professionals, organizations and nursing leaders should train nurses on essential cybersecurity issues and safeguards, making it an essential 2024 nursing trend. They should also maintain compliance with Health Insurance Portability and Accountability Act (HIPAA) standards and review their current protocols to ensure they have robust defense measures.
21. Automation Will Free Nurses to Tackle More Complex Challenges
Nurses carry out repetitive tasks each day in service of their patients. These tasks can be physically demanding and monotonous when completed hundreds of times per shift. Robots and other automation tools are increasingly used to handle basic jobs in clinical settings.
Moxi is a self-operating robot that delivers medical supplies to exam rooms in several Texas hospitals. Henry Ford Health System deploys Xenex LightStrike robots to disinfect surfaces with ultraviolet-C (UV-C) after exams and in-patient stays. Brigham and Women's Hospital uses Boston Dynamics robots to measure the vitals of COVID-19 patients.
The future of nursing will see robots increasingly involved in diagnostics and procedures. In 2024, nurses may share the halls with robot colleagues that ease their workload. Additionally, nurses will increasingly turn to machine learning and artificial intelligence (AI) to help automate mundane and repeatable tasks, freeing more time for direct patient care.

22. There Will Be a Growing Role for Nurses in Health Equity Efforts
The Centers for Disease Control and Prevention (CDC) defines the term "health equity" as "everyone has a fair and just opportunity to attain their highest level of health." Millions of patients face inequities due to one or more social determinants of health, including the following:
- Housing insecurity
- Lack of access to healthy food
- Racial discrimination
- Poor air and water quality
Nurses encounter the consequences of these determinants in their daily work. Social and economic inequalities were magnified by the COVID-19 pandemic, leaving front-line health workers to find solutions for their patients.
The NAM sees opportunities for health equity innovations by nurses. In its report The Future of Nursing 2020-2030, the NAM advocates for health care providers to "incorporate nursing expertise in designing, generating, analyzing, and applying data" into health equity programs. Nursing professionals will have opportunities to improve conditions for patients in 2024 and beyond.
23. Support for Nurses' Mental Health Will Grow
Given the physical and emotional demands of the nursing profession, burnout is a significant risk. The rate of nurses leaving the profession bears this out and makes rising mental health awareness another key nursing trend for 2024 and beyond.
Nurse leaders can advocate for their own mental well-being and that of their team members in many ways. Examples are as follows:
- Investing in AI and other tools to help nurses bear their workload
- Promoting more flexible scheduling, including ample time off
- Providing on-site support and counseling options for nurses to opt into
The bottom line: Successful nurses will need to be mindful of their own mental health concerns, in 2024 and into the future.

24. Preventative Care Will Be Prioritized
Nurses and other health care professionals will continue to prioritize preventative measures in holistic care in 2024. This involves addressing potential health issues before they arise. Preventative measures include:
- Performing risk assessments
- Providing health education and community outreach
- Administering vaccinations
- Encouraging screenings and other early detection tests
- Facilitating chronic disease management
With effective prevention, patients can mitigate the risk of developing a serious or chronic illness before it happens, avoiding extra health care visits and decreasing the likelihood of chronic pain and discomfort.
Stay Ahead of Nursing Trends
As an FNP, you can bridge gaps in primary care. You'll experience a transformative education at Carson-Newman through our online MSN-FNP or online Post-Master's FNP Certificate programs.
Why become an FNP student at Carson-Newman? Our FNP students benefit from these distinctive Carson-Newman advantages:
- Online coursework with no mandatory login times, so you can continue working full time or part time as you study
- Small-sized classrooms to accommodate your learning needs
- Ongoing clinical placement services, so you can focus on your studies and maintain a work-study-life balance
- A dedicated student success advisor who'll support you from start to finish
NP was ranked No. 1 in Best Health Care Jobs by U.S. News & World Report in 2022. As an NP, you'll empower your career as a holistic leader in primary care.
Learn more about our online MSN-FNP or online Post-Master's FNP Certificate programs.